Abstract
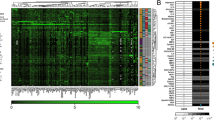
The quest for reliable biomarkers of systemic lupus erythematosus (SLE) nephritis is an area of intense contemporary research. In this study, surface-enhanced laser desorption/ionization time-of-flight mass spectrometry (SELDI-TOF-MS) technology was used for urinary proteomic profiling of patients with SLE nephritis. Clinical, laboratory, and kidney biopsy data from pediatric patients with SLE (n = 32) were analyzed. Children with juvenile idiopathic arthritis (n = 11) served as controls. SELDI-TOF-MS was performed using ProteinChips with different chromatographic surfaces. The resulting spectra were analyzed with Bio-Rad Biomarker Wizard software. A consistent urinary proteomic signature for SLE nephritis was found, comprising eight biomarker proteins with peaks at m/z of 2.7, 22, 23, 44, 56, 79, 100, and 133 kDa. The peak intensities of these biomarkers were significantly greater in patients with SLE nephritis compared with controls and SLE patients without nephritis. These biomarkers were strongly correlated with renal disease activity and moderately with renal damage. For the diagnosis of active nephritis, the area under the receiver operating characteristic curve was ≥0.90 for 22, 23, 44, 79, and 100 kDa biomarkers. Thus, SELDI-TOF-MS has identified a urine proteomic signature strongly associated with SLE renal involvement and active SLE nephritis.



Similar content being viewed by others
References
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40:1725
Ho A, Barr SG, Magder LS, Petri M (2001) A decrease in complement is associated with increased renal and hematologic activity in patients with systemic lupus erythematosus. Arthritis Rheum 44:2350–2357
Schiffenbauer J, Hahn B, Weisman MH, Simon LS (2004) Biomarkers, surrogate markers, and design of clinical trials of new therapies for systemic lupus erythematosus. Arthritis Rheum 50:2415–2422
Cutillas P, Burlingame A, Unwin R (2004) Proteomic strategies and their application in studies of renal function. News Physiol Sci 19:114–119
Gunawardana CG, Diamandis EP (2007) High throughput proteomic strategies for identifying tumor-associated antigens. Cancer Lett 249:110–119
Hewitt SM, Dear J, Star RA (2004) Discovery of protein biomarkers for renal diseases. J Am Soc Nephrol 15:1677–1689
Nguyen MT, Ross GF, Dent CL, Devarajan P (2005) Early prediction of acute renal injury using urinary proteomics. Am J Nephrol 25:318–326
Schaub S, Wilkins J, Weiler T, Sangster K, Rush D, Nickerson P (2004) Urine protein profiling with surface-enhanced laser-desorption/ionization time-of-flight mass spectrometry. Kidney Int 65:323–332
Petty RE, Southwood TR, Manners P, Baum J, Glass DN, Goldenberg J, He X, Maldonado-Cocco J, Orozco-Alcala J, Prieur AM, Suarez-Almazor ME, Woo P (2004) International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2001. J Rheumatol 31:390–392
Gladman DD, Ibanez D, Urowitz MB (2002) Systemic lupus erythematosus disease activity index 2000. J Rheumatol 29:288–291
Brunner HI, Feldman BM, Bombardier C, Silverman ED (1999) Sensitivity of the Systemic Lupus Erythematosus Disease Activity Index. British Isles Lupus Assessment Group Index, and Systemic Lupus Activity Measure in the evaluation of clinical change in childhood-onset systemic lupus erythematosus. Arthritis Rheum 42:1354–1360
Hay EM, Bacon PA, Gordon C, Isenberg DA, Maddison P, Snaith ML, Symmons DP, Viner N, Zoma A (1993) The BILAG index: a reliable and valid instrument for measuring clinical disease activity in systemic lupus erythematosus. Q J Med 86:447–458
Gladman DD, Goldsmith CH, Urowitz MB, Bacon P, Fortin P, Ginzler E, Gordon C, Hanly JG, Isenberg DA, Petri M, Nived O, Snaith M, Sturfelt G (2000) The Systemic Lupus International Collaborating Clinics/American College of Rheumatology (SLICC/ACR) Damage Index for Systemic Lupus Erythematosus International Comparison. J Rheumatol 27:373–376
Weening JJ, D’Agati VD, Schwartz MM (2004) The classification of glomerulonephritis in systemic lupus erythematosus revisited. Kidney Int 65:521–530
Churg J, Bernstein J, Glassock RJ (1995) Renal disease: classification and atlas of glomerular diseases, 2nd edn. Igaku-Shoin, New York
Brunner HI, Mueller M, Rutherford C, Passo MH, Witte D, Grom A, Mishra J, Devarajan P (2006) Urinary neutrophil gelatinase-associated lipocalin as a biomarker of nephritis in childhood-onset systemic lupus erythematosus. Arthritis Rheum 54:2577–2584
Hanley JA (1989) Receiver operating characteristic (ROC) methodology: the state of the art. Crit Rev Diagn Imaging 29:307–335
Oates JC, Varghese S, Bland AM, Taylor TP, Self SE, Stanislaus R, Almeida JS, Arthur JM (2005) Prediction of urinary protein markers in lupus nephritis. Kidney Int 68:2588–2592
Varghese SA, Powell TB, Budisavljevic MN, Oates JC, Raymond JR, Almeida JS, Arthur JM (2007) Urine biomarkers predict the cause of glomerular disease. J Am Soc Nephrol 18:913–922
Gudehithlu KP, Pegoraro AA, Dunea G, Arruda JA, Singh AK (2004) Degradation of albumin by the renal proximal tubule cells and the subsequent fate of its fragments. Kidney Int 65:2113–2122
Strong KJ, Osicka TM, Comper WD (2005) Urinary-peptide excretion by patients with and volunteers without diabetes. J Lab Clin Med 145:239–246
Mosley K, Tam FW, Edwards RJ, Crozier J, Pusey CD, Lightstone L (2006) Urinary proteomic profiles distinguish between active and inactive lupus nephritis. Rheumatology (Oxford) 45:1497–1504
Li Y, Tucci M, Narain S, Barbes EV, Sobel ES, Segal MS, Richards HB (2006) Urinary biomarkers in lupus nephritis. Autoimmun Rev 5:383–388
Acknowledgement
This study is supported by a clinical research grant NIAMS P60 AR47784. Dr. Brunner is supported by a grant from the Alliance for Lupus Research and the CCHMC Translational Research Initiative. Dr. Devarajan is supported by grants from the NIH/NIDDK (RO1-DK53289, P50-DK52612, R21-DK070163). Dr. Wiers is supported by T32 AR007594 and the NIH Loan Repayment Program. We are indebted to our clinical coordinators Jamie Meyer-Eaton and Cynthia Rutherford for their assistance, Lukasz Itert for the data management, the NIAMS Tissue Repository (director Susan Thompson; AR047363) for the sample management, Alison Kissling for her technological support with the manuscript preparation, and to our patients and families for their participation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Suzuki, M., Ross, G.F., Wiers, K. et al. Identification of a urinary proteomic signature for lupus nephritis in children. Pediatr Nephrol 22, 2047–2057 (2007). https://doi.org/10.1007/s00467-007-0608-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-007-0608-x